
A 30-year-old woman with a sore throat thought she had a common winter bug, and went on holiday to Porto, then ended up in intensive care for 10 days in an induced coma. Jennifer Gavin was left close to death when her sore throat rapidly escalated into life-threatening sepsis caused by severe pneumonia.
After being initially misdiagnosed with flu, she was admitted to A&E and spent three weeks in hospital, including 10 days in ICU. Doctors later told her she likely would not have survived had she not returned to hospital when she did. Jennifer, originally from Greenock, Scotland, but now living in London, was fit and active, playing netball up to five times a week.
“I was living a very normal and average life of a 30-year-old woman in London, spending my week working full time as a change manager and weekends socialising with friends, travelling around Europe and living an active lifestyle,” said Jennifer. “I am an avid netballer, and the summer before I was sick I was playing netball five times a week and coaching primary school kids how to play.

“I was really happy in life the summer of 2024, and would probably class it as one of my favourite summers that I've had while living in London.”
When she began to develop a sore throat in September 2024, she wasn’t concerned at all. “My work colleagues and friends all had sore throats and colds around the same time I started feeling unwell, so I genuinely thought nothing of it,” Jennifer said. “I was flying to Porto for the weekend to celebrate my birthday the night that my throat started feeling sore, and it was only when I reached the airport that I started feeling achy and really tired.
“By the time I landed in Porto my whole body was in pain and I assumed I had the flu.”
Jennifer’s mum had once had sepsis, and the thought did cross her mind that her developing symptoms could be a sign of something more serious. In Porto, she Googled sepsis symptoms as her shivering and sweating had gone up a level. But because she could still urinate as normal, she convinced herself it wasn’t sepsis.
Back in the UK, Jennifer went to the GP as she has Crohn’s Disease and is immunosuppressed. “I thought it could be more serious as I just wasn't getting any better and I believed that I was dehydrated,” Jennifer said. “The GP suspected I had flu and I was sent home for bed rest.”
- 'I'm a cardiologist and there are three things I would never eat or drink'
- ‘Midwives said it was a panic attack - two days later I was in coma and baby was dying’
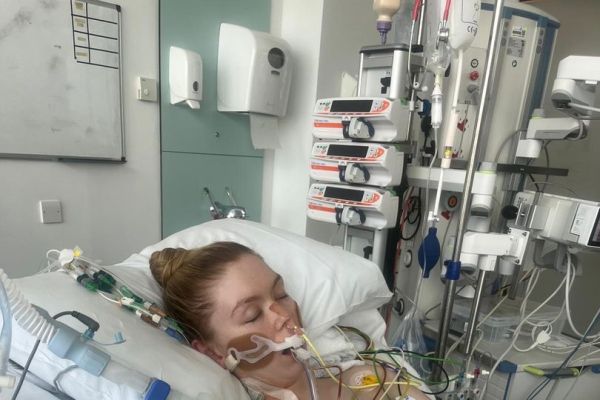
A few days later, on the evening of Friday September 13 Jennifer could hear her heart pounding in her chest. She wasn’t feeling any better so she decided to pick the phone up and call 111. The operator said as she had had a persistent fever for over a week she should go to A&E, which saved her life.
“When I got to A&E and was admitted to Resus, the doctor looked at me and said I was very lucky that I came in as I probably wouldn't have survived the night,” Jennifer said. “That was the first time I knew something serious was happening, and my family caught the first flight to London Saturday morning to be at my side.”
When she was first admitted, doctors disagreed over what was wrong with her. It went from gallbladder issues, to a Crohn’s disease flare, to hepatitis. “I now understand this is because sepsis was affecting all my organs and making it difficult to understand where the infection started, which slowed down my treatment plan,” Jennifer said.
“Eventually, I was told I had pneumonia, and in one way it was a relief because I knew what that was, I was young and fit and thought it was easily treatable. Dealing with a diagnosis of pneumonia compared to a diagnosis of sepsis was very different, and it wasn't until day two that they said I was septic.
“This caused a lot of distress for me, as immediately sepsis becomes so much more serious than pneumonia, and I knew how lucky my Mum was to survive it. It also made me wish I had trusted myself sooner to go to the hospital. It was a big lesson for me in trusting instincts and advocating for myself.”
Jennifer’s treatment consisted of a 10-day ICU stay, six days in a ventilated coma, countless variations of IV antibiotics due to not knowing what was causing the infection, a chest drain to drain litres of fluid that had collected in her pleural cavity, and a further nine days in hospital.
Blood cultures on day three of her coma discovered that the bug in her blood was Fusobacterium necrophorum, which is usually a an infection that causes severe sore throats. Jennifer didn't really have time to process what was happening due to delirium and had to begin processing the traumatic experience when she woke up from her coma.
Jennifer wants to raise awareness of the danger of sepsis, especially how it can manifest differently in different people. “I wish people knew how quickly things can change, and that the faster you get help for symptoms the greater chance you have of recovering,” she says.
“Also, I wish people would trust themselves more and advocate for themselves when they do not think they are getting better, even if they have had a medical opinion during the illness period. Sepsis can affect anyone, and I think me presenting as a fit, young woman perhaps delayed proper treatment.
“I put this into action when I had sepsis for a second time in May 2025 because I noticed the signs quicker: my heart rate was fast, my temperature was elevated, I was achy and sore and I was vomiting. I went to the hospital as soon as I landed back in the UK and I was put on IV antibiotics for Urosepsis. This was an overnight admission followed by oral antibiotics compared to the first ordeal that I went through, all because I sought help quicker and trusted that I knew something was wrong with my body.”
She wants to raise awareness that sepsis can affect young, fit people and that trusting your instincts and seeking repeat medical help can save lives.
Jennifer’s motivation is personal: even though her mum had also survived sepsis, Jennifer still did not recognise the symptoms in herself because of how differently the symptoms can manifest. “I feel really strong and lucky to be here, knowing the outcome could have been very different,” says Jennifer.
“My life is pretty much back to normal, but I don't think a day will go by that I don't think about what happened. It has changed me forever but in the best way. I'd like to think that I don't get as stressed about silly things as it has given me a lot of perspective, and it has also been a great motivator for anything hard in life.
“I just think back to being in the hospital room, freshly out of the coma and know if I can recover from that I can do anything. Approximately 48,000 people die each year in the UK from sepsis, which equates to five people every hour. And that number is growing.
In April Jennifer will run the London Marathon to raise money for Sepsis Research FEAT, the UK's leading sepsis research charity. “Sepsis Research FEAT is the UK's only sepsis research charity, and it's so important to me to continue to not only raise awareness of sepsis, but raise vital funds to ensure that more research can be done to understand sepsis and the treatments for it so that more people can survive,” she says.
“I've decided to run the London Marathon 2026 for Sepsis Research FEAT, excitingly the first time the charity has had a place in the race. This is not only for myself, and to prove just how far I've come (the thought of using the same lungs that were so damaged I required a ventilator, to power me through the London marathon is an incredible thought!), but it's for all those people who weren't as lucky as I was.
“'Do it for those that can't' will be written on my hand on the day to remind myself of the seriousness of sepsis and the awareness that still needs to be done around it.”
Donate to Jennifer’s fundraiser at: https://2026tcslondonmarathon.enthuse.com/pf/jennifer-gavin
Contact to : xlf550402@gmail.com
Copyright © boyuanhulian 2020 - 2023. All Right Reserved.